Overview
This website does not in any way support the self administration of ibogaine nor does it consider itself medically qualified to pass judgement on the suitability of any one person for ibogaine treatment. A proper medical evaluation is required in line with the safety manual as a minimum.
CLICK BELOW TO EXPAND GRAPHIC:
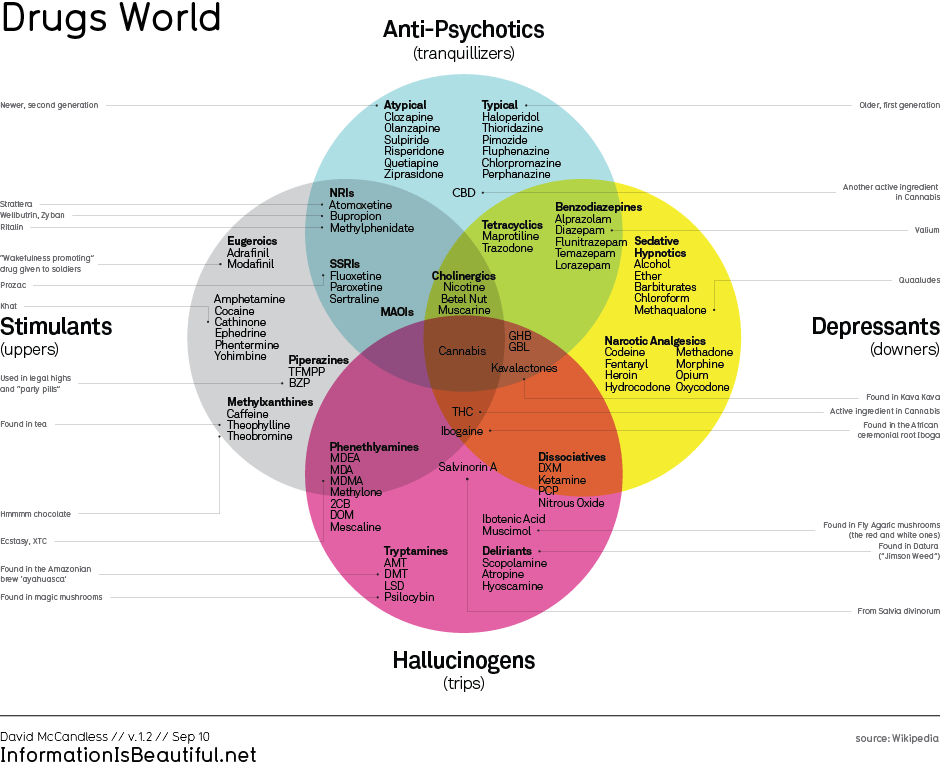
Opioids
Under no circumstance can a treatment commence until sufficient time has passed since the last use of an opioid. In the case of heroin the minimum is 8 hours. For morphine, 24 hours. And for methadone the client should have switched to a shorter acting opioid such as heroin or morphine, at a minimum 5 (24 hour) days earlier. The use of an opioid during a session will lead to a potential death as ibogaine resets the brains opioid tolerance.
Alcohol
Alcohol dependence is treated where the client has abstained for at least 1 month. However it is necessary to use a benzodiazepine such as klonopin which is specifically known for its ability to interrupt seizures more successfully than other benzodiazepines and is often prescribed as an adjunct medication for epilepsy patients. The risk with alcohol of seizures is not high but it can be minimised with the use of an anti-seizure medication during the session.
Stimulant Dependence
Ibogaine can also successfully interrupt stimulant addictions, mainly through its ability to modulate the release of dopamine in the brain and “reset” countless other neurochemical pathways, many of which are still not yet understood. Withdrawals from cocaine and crack are usually not physical; they are generally “mental” in the sense of the addict experiencing intense anxiety, sleeplessness, and constant cravings for their drug. Because stimulant dependence is mainly connected to the release of the neurotransmitter dopamine, ibogaine interrupts these “mental” withdrawal symptoms through its action on the dopamine pathways, changing the way dopamine is released.
Methamphetamine, when used heavily, can cause a physical withdrawal syndrome.
Benzodiazepines
Reports on the ground indicate that ibogaine does not reset tolerance to benzodiazepines. However it seems the original Indra extract does and it may be resonable to speculate by extension that a properly prepared extract of iboga will also do the same as both consists of the many alkaloids in the iboga plant. However, there are many different extracts and from anecdotal reports some do not appear to work.
There is always a risk of seizures when withdrawing from benzodiazepines. During withdrawal, the risk of seizures increases by the size of the tolerance. For example, a person dependent on 3mg of xanax per day is much less likely to have a seizure during treatment than a person dependent on 10mg xanax per day.
Benzodiazepine-dependent individuals may try a variety of methods to avoid the risk of seizures. For example, lowering tolerance slowly before treatment would decrease seizure risk. Also, some ibogaine treatment providers suggest that small doses of a benzodiazepine be given during the treatment as needed to prevent seizures.
